Do you want to be part of a team championing health rights for all West Australians?
Position Title: Operations and Impact Manager
Location: Mount Lawley, WA
Work Type: Full-time/Part-Time
Level: SCHADS L7
Salary: $60.27-$62.79/hour + Superannuation
About us
We are the Health Consumers’ Council WA (HCCWA). We work to make sure that the voices of West Aussies are heard and acknowledged in healthcare system matters. We fight for an equitable system that is shaped for the people of WA.
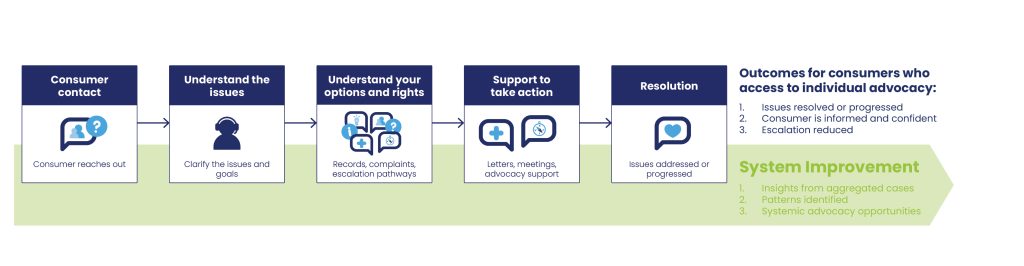
This role exists to strengthen organisational effectiveness by managing operations, streamlining systems, improving knowledge flow, and ensuring operational infrastructure frees up staff time to enable people to focus on the relational high impact work of consumer advocacy and engagement. The role sits at the centre of the organisation, connecting strategy, operations (including finances, HR and facilities) and delivery.
About you
- Demonstrated experience improving systems, processes, and organisational effectiveness in a complex or not-for-profit environment
- Strong operational knowledge across finance, HR, governance, and compliance, with the ability to translate strategy into practical outcomes
- Highly organised with excellent analytical and problem-solving skills, able to manage competing priorities and drive work through to completion
- Collaborative and influential communicator, with a proactive, hands-on approach and a commitment to continuous improvement
About the position
This pivotal role sits at the centre of the organisation, connecting strategy, operations, and delivery to strengthen overall effectiveness and impact. As the Operations and Impact Manager, you will lead the development and continuous improvement of systems, processes, and operational infrastructure—ensuring staff are supported to focus on high-value consumer advocacy and engagement work.
Working closely with the Executive Director and Leadership Team, you will oversee key operational functions including finance, HR, IT, and governance, while driving efficiency, consistency, and best practice across the organisation. You will play a critical role in enabling organisational performance by improving knowledge flow, embedding practical systems, and supporting teams to deliver priority work effectively.
This is a hands-on and strategic role suited to someone who thrives in a dynamic, purpose-driven environment and is passionate about improving how organisations operate to achieve meaningful outcomes for the community.
View the position description here.
A typical week might see you
- Leading and progressing operational priorities across finance, HR, IT, and governance to ensure the organisation runs efficiently and effectively
- Working closely with the Executive Director and Leadership Team to implement strategic and operational plans
- Reviewing and improving systems and processes to reduce administrative burden and enhance organisational performance
- Coordinating with external providers (finance, HR, IT) to ensure high-quality, compliant, and value-for-money services
- Supporting teams to deliver priority work, streamline workflows, and adopt improved ways of working
- Overseeing key governance activities, including policy development, compliance tracking, and Board support
The role offers you
- The opportunity to be a part of a workplace that is driven by championing West Aussie consumer health rights
- A welcoming, inclusive and supportive workplace, where everyone is encouraged to bring all of themselves
- A competitive not-for-profit annual base salary with salary packaging
- Flexible working arrangements including the opportunity to work from home occasionally
- Additional leave entitlements
Diversity and inclusion
At Health Consumers’ Council WA we know that strength comes from diverse perspectives being at the table. We particularly encourage applications from Aboriginal and Torres Strait Islander people, people from culturally diverse backgrounds and identities, people with disability and LGBTIQA+ community members.
Selection Criteria
Essential
- Demonstrated experience improving organisational systems, processes, and overall effectiveness in a complex environment
- Strong operational knowledge across finance, HR, governance, and compliance, including the ability to interpret financial reports
- Proven ability to lead and deliver complex projects, manage competing priorities, and drive outcomes to completion
Desirable
- Demonstrated interest in health advocacy or experience working in a values-driven or community-based organisation
- Experience using CRM systems (e.g. Microsoft Dynamics) to support organisational operations and reporting
- Understanding of governance, compliance, and risk frameworks within a not-for-profit environment
- Experience supporting organisational growth, including income diversification or fee-for-service delivery initiatives
How to apply
Provide a cover letter of no more than two (2) pages addressing the selection criteria, along with a current resume outlining your work experience, skills and any relevant education or training to Clare Mullen, our Executive Director at jobs@hconc.org.au clearly stating which role you’re applying for.
Applications that do not address the selection criteria may not be considered.
Applications close Wednesday, 17 June 2026 at 8am
If you require any adjustments to submit your application or wish to have a confidential discussion about the role, please contact Tania Harris, Engagement and Advocacy Manager on (08) 6109 6709